Is HRV the Canary in the Coalmine?
- Shaun Kober

- Apr 3
- 17 min read
Updated: Apr 10
What my own health data showed before a spinal infection was diagnosed — and why understanding heart rate variability can act as an early warning system.
The phrase “canary in the coalmine” comes from coal mining, where canaries were taken underground as an early warning system. The bird itself was not the focus. It was the signal that the toxic gases in the environment had become dangerous before the full consequences were obvious to the miners.
That analogy fits heart rate variability remarkably well.
HRV is not a diagnosis. It does not tell you exactly what is wrong, where it is wrong, or how serious the issue is in isolation. But it can provide an early indication that the organism is under strain, that recovery capacity is being compromised, and that the autonomic nervous system is shifting in response to stressors that may not yet be fully understood.
In performance settings, HRV is often discussed in relation to training load, recovery status, sleep quality, travel, psychological stress, illness, and readiness. Used properly, it is less useful as a standalone number and more useful as part of a broader pattern-recognition process. When HRV trends downward, especially alongside deteriorations in sleep, energy, mood, and physical output, it should prompt closer attention. Not panic, but investigation.
That is why my recent experience reinforced the way I think about these metrics.
Before I had a formal diagnosis, before the full severity of the situation was clear, and before I began antibiotic treatment, my health data was already showing that something was wrong. HRV had fallen dramatically away from its previous baseline. Sleep quality deteriorated. Recovery markers shifted. At the time, those changes in data (and the pain I was feeling) couldn't be explained away as stress, accumulated fatigue, poor sleep, or the normal consequences of hard training and life load.




They were not random fluctuations.
They were early signs that my system was allocating resources toward a deeper physiological problem. In my case, that problem was a spinal infection that went untreated for three weeks.
Looking back, I believe I was fortunate in two ways. First, the metrics were signalling that my internal environment had changed dramatically well before the situation was fully understood. This prompted me to follow up when I wasn't happy with being sent home from the emergency department after a week of escalating pain and poor metrics. Second, I was starting from a relatively healthy baseline, which may have bought me time while the infection developed without treatment.
This article is not an argument that HRV can diagnose infection.
It cannot.
It is an argument that HRV can function as an early warning signal. A canary in the coalmine. A marker that the organism is no longer operating within its normal range, and that something deeper may require attention.
For coaches, athletes, and everyday people alike, that distinction matters. Because the value of data is not in pretending it gives certainty. The value is in recognising when the pattern changes enough to ask better questions, investigate earlier, and respond before a manageable issue becomes a major one.
What Heart Rate Variability Actually Reflects
HRV refers to the variation in time between successive heart beats.

That point is important, because many people assume a healthy system should behave like a metronome. In reality, a well-regulated organism does not produce perfectly even intervals between beats. It continually adjusts moment to moment based on internal and external demands. The greater that adaptive capacity, the more variability tends to exist within a healthy context.
At a physiological level, HRV is commonly used as a non-invasive window into autonomic nervous system behaviour.
Broadly speaking, the autonomic nervous system helps regulate the balance between:
Sympathetic activity — mobilisation, alertness, threat response, energy expenditure
Parasympathetic activity — recovery, restoration, digestion, repair, energy conservation
This is often oversimplified as “fight or flight” versus “rest and digest”, but real physiology is more dynamic than that. These systems are not simply on or off. They are constantly interacting, adapting, and reallocating resources based on what the organism perceives it needs to do in order to survive and function.
That is where HRV becomes useful.
A higher HRV does not automatically mean a person is healthier in every context, just as a lower HRV does not automatically mean something is seriously wrong. What it often reflects is the current state of regulatory flexibility. In simple terms, how much room the system appears to have to adapt.
When the body is well recovered, sufficiently fuelled, sleeping well, and not under excessive strain, HRV will often sit closer to an individual’s normal upper range. When the body is under load, whether from hard training, psychological stress, poor sleep, travel, dehydration, inflammation, illness, or a combination of stressors, HRV will often trend downward, which is the reflection of the organism changing its priorities.
If the body detects threat, instability, tissue damage, infection, or rising physiological cost, it begins reallocating energy and attention toward immediate survival and restoration. Recovery capacity narrows. Readiness tends to fall. Sleep can deteriorate. Resting heart rate may rise. Motivation, mood, output, and tolerance for training often shift with it.
From a coaching perspective, this is why HRV should be understood as a systems marker, not just a heart marker.
It is influenced by the heart, but it reflects much more than cardiovascular fitness alone. It is shaped by the interaction between the nervous system, immune system, endocrine system, metabolic state, behavioural inputs, and total life load. Training stress matters, but so do illness, emotional strain, disrupted sleep, under-fuelling, and inflammation. The body does not separate these neatly just because we want clean data.
This is also why context matters so much.
A single HRV reading has limited value in isolation. What matters more is the pattern relative to the individual’s baseline. What has been normal for them? What has changed? What else changed at the same time? Did sleep fall away? Did resting heart rate rise? Did soreness linger? Did motivation drop? Did the person suddenly feel flat, anxious, wired, or unusually fatigued?
That broader pattern is where HRV becomes meaningful.
In practical terms, HRV is best viewed as an indicator of how costly life currently is for the organism.
When that cost rises, variability often falls.
Sometimes the cause is obvious: a brutal training block, poor sleep, travel fatigue, calorie restriction, or emotional stress. Sometimes the cause is less obvious. That is where people need to pay attention, because unexplained suppression in HRV, especially when it persists and coincides with other red flags, may indicate that the body is dealing with more than just normal training fatigue.
That was the lesson in my case.
The metric itself did not diagnose the problem. But it did reflect that the organism was no longer behaving as expected. Something had changed. The system was under massive pressure. And in hindsight, the data was showing that well before the full clinical picture had caught up.
The key point is this:
HRV reflects regulation, adaptability, and physiological cost.
It is not a crystal ball. It is not a diagnosis. But it is often a very useful signal that the organism is either coping well or starting to lose room to manoeuvre.
From there, the smartest question is not, “What is my HRV today?”
The smartest question is:
What is this trend suggesting about the current state of the system?
Why HRV Is Useful — And Where People Get It Wrong
In performance settings, HRV can be a valuable tool because it gives us a repeatable, non-invasive way to monitor how the organism is responding to total stress load. Not just training load, but life load in the broadest sense. It offers a window into whether the system appears to be absorbing stress, adapting to it, or struggling under it.
Used well, HRV helps identify trends such as:
accumulating fatigue
inadequate recovery
poor sleep tolerance
excessive sympathetic load
reduced readiness to perform
potential early signs of illness or systemic strain
That does not mean HRV tells us why those things are happening.
It means HRV can alert us that something has shifted.
This is where many people get it wrong. They want HRV to behave like a diagnostic label. They want one number to tell them whether they should train, rest, panic, push harder, or assume they are getting sick. That is not how useful coaching metrics work.
HRV is not valuable because it gives perfect answers. It is valuable because it improves the quality of the questions.
If an athlete’s HRV drops for one day after a hard session, that may be entirely normal. If it rebounds quickly and the athlete feels good, sleeps well, and performs well, there may be no issue at all. In fact, temporary suppression can simply reflect that training imposed a meaningful demand.
But if HRV remains suppressed for several days, sleep quality worsens, resting heart rate rises, mood drops, and the athlete starts feeling flat, wired, sore, or unusually fatigued, then the pattern becomes more meaningful. At that point, the conversation shifts from “What does this number mean?” to “What is driving this broader response?”
That is the correct use of the metric.
From a coaching standpoint, HRV works best when it is placed inside a decision-making framework that includes context. Training load. Sleep duration and quality. Travel. Nutrition. Illness symptoms. Psychological stress. Motivation. Performance output. Subjective feel. In other words, the metric becomes more useful as part of a system, not as a replacement for one.
Another common mistake is assuming that higher is always better.
It is not that simple.
A chronically low HRV relative to baseline may suggest excessive stress, poor recovery, illness, or reduced autonomic flexibility. But an unusually high reading is not automatically a green light either. In some contexts, unusually elevated HRV can occur during maladaptation, parasympathetic overreaching, or during periods where the body is not mounting its normal response in the way you would expect. The key issue is not whether the number is high or low in absolute terms. The key issue is whether it is normal or abnormal for that individual, in that context, relative to their recent pattern.
That is why baseline matters so much.
HRV is deeply individual. One person’s normal may be another person’s warning sign. Comparisons between people are far less useful than comparisons against your own established trend. The question is not whether your HRV looks impressive on paper. The question is whether it is behaving in a way that is consistent with your normal physiology, current demands, and overall state.
There is also a behavioural trap that comes with HRV.
Some people become too reactive to the data. They wake up, check the score, and let that number dictate their mindset before the day has even begun. That can become counterproductive very quickly. A metric that is meant to improve awareness can end up increasing anxiety and reducing trust in one’s own perception.
That is not better coaching. It is just a new form of dependence.
The solution is to use HRV as a guide, not a ruler. It should inform judgement, not replace it. A low reading might suggest the need to zoom out, assess the bigger picture, and potentially adjust the day. It should not automatically trigger fear. Equally, a normal reading should not overrule obvious symptoms, poor function, or mounting red flags.
This becomes especially important in relation to illness.
HRV can often register that the body is under strain before symptoms become severe or before a diagnosis is made. That is one of the reasons it can be so useful. But it cannot tell you whether the problem is a virus, bacterial infection, overreaching, emotional stress, under-fuelling, inflammation, poor sleep, or some combination of all of the above. The signal may be real, but the interpretation still requires thought.
That is the balance coaches and athletes need to understand.
HRV is useful because it can highlight that the organism is paying a cost.
In that sense, HRV sits in the same category as many good performance metrics: powerful when interpreted intelligently, misleading when stripped of context, and dangerous when people start asking it to do more than it was ever designed to do.
My experience reinforced that point in a very real way.
The data did not diagnose my spinal infection. It did not tell me where the issue was. It did not replace imaging, bloods, or medical assessment. But it did show that my system had moved away from its normal state and was not recovering the way I would expect it to, given the circumstances.
That matters.
Because when a marker like HRV shifts sharply, stays suppressed, and lines up with injury or pain, deteriorating sleep, reduced resilience, and unusual symptoms, the smartest response is not to obsess over the score.
It is to recognise that the canary is no longer singing.
My Timeline: How The Data Shaped My Actions
On the 5th of February I went for a light jog to warm up before a longer planned run. My calf locked up. I stopped, stretched without resolve, walked home, and thought I’d try again later.
A few hours passed before the onset of pain and upper/middle back spasms began.
I went to bed to try and sleep it off and barely got out of bed for the next few days.
I couldn’t point to a clear mechanism of injury. The only thing that came to mind was being caught in a guillotine choke the night before during an MMA sparring session, but it didn’t seem significant enough to explain what I was feeling.
What did stand out was my data.

From that point on, the trend was hard to ignore. HRV dropped hard. Sleep deteriorated. Stress climbed. Resting heart rate shifted. Activity collapsed. The system was clearly under massive pressure.
At that stage, I didn’t know I had a spinal infection.
But my body knew something was wrong.
And my wearable data was reflecting it almost immediately.
The First Trip To Emergency
After about a week of pain and increasingly concerning changes in my metrics, I went to the emergency department.
I explained my symptoms. I showed them the data from my wearable. I tried to give context around what was normal for me and how sharply things had changed.
After roughly seven hours in two different chairs, I was sent home with a prescription for ten painkillers and told to move more, breathe deeper, and follow up with a GP in a week if things didn’t improve.
That was difficult to accept, because I knew something was wrong.
Not because a wearable had diagnosed me. It hadn’t.
But because my symptoms and my baseline-to-current shift were telling the same story: this was not normal.
The Diagnosis Took Time And Treatment Was Delayed
The next day, through my network, I spoke with a GP who took the situation seriously and referred me for an MRI.
That MRI led to a follow-up call and a request for a CT scan and blood tests, with suspected spinal fracture initially on the table. All up, these actions took another eight days.
Then came another call.
This time, the concern was infection. There appeared to be a collection of fluid in or around the spine, and I was told to return to emergency.
So I did.
I spent another 12 hours in two different chairs, speaking to multiple people, repeating the story again, before finally being admitted for further testing.

That was on Saturday 21st of February.
I didn’t go for another MRI until Tuesday night.
Two days later, I had a CT scan and biopsy.
Broad-spectrum antibiotics began that night.
Three full weeks after the initial onset of pain.
Three weeks after a dramatic and sustained crash in my health metrics.
Three weeks after my system had already been waving a red flag.
The Slow Road Back
In total, I spent ten days in hospital before moving into the Hospital in the Home program, where a nurse visited every day to administer IV antibiotics.
Slowly, the metrics began to stabilise.
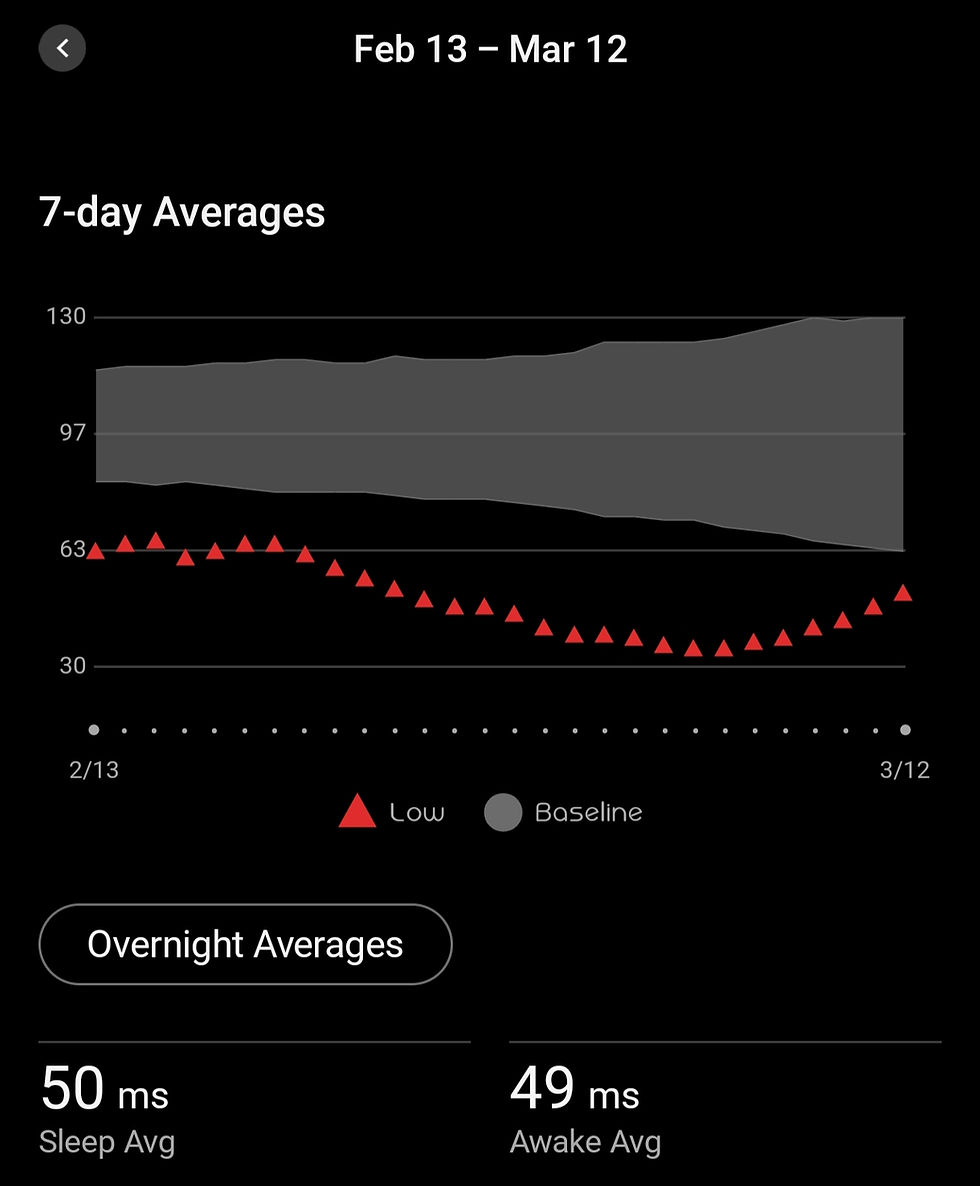
The symptoms eased. The data shifted. The antibiotics were doing what they needed to do, and my system began the long process of stabilising ahead of recovery.
I completed four weeks of IV antibiotics and have since moved onto another eight weeks of oral antibiotics.
As I write this, eight weeks into the process, I’m functioning at roughly 70 percent.
I've returned to the gym this week to rebuild function. What used to be my warm-up is now my workout.
Even that has to be scaled back.
Going from around 15,000 steps a day to barely able to hit 500 (many of them slow and laboured) is a humbling way to learn what capacity really means.
What Surprised Me About Medicine
As a performance coach, I’ve used HRV data with professional athletes for years.
In training camps and high-pressure environments, it helps inform load, recovery, and timing. It helps us avoid pushing too hard too soon and peaking at the wrong time. It helps us see when the system is coping and adapting and when it is starting to lose room to move.
The goal is never to chase perfect numbers. The goal is to understand readiness, recovery, and risk. If an athlete is drifting too far from baseline, you adjust before the wheels fall off.
That’s what struck me most during this experience.
In performance settings, context matters. Baseline matters. Trends matter.
In the medical setting, at least in my case, that same context was largely ignored.
That was disappointing, especially since the concerns turned out to be valid.
I understand that emergency departments have to make decisions based on the information in front of them at the time. I also understand that wearable data sits outside the traditional medical model and may not carry much weight in an acute care setting.
But from the patient’s side of the experience, it is hard to ignore how frustrating it feels when the canary is clearly struggling, and nobody yet believes the air is dangerous.
I’m not arguing that emergency departments should diagnose serious infections from a smartwatch.
They shouldn’t.
But I do think we are missing something when patient-generated data is dismissed entirely.
The Missed Opportunity In Medicine
This is where I think modern healthcare still has a blind spot.
Healthcare is excellent when it identifies established pathology. It is very good at confirming what is already serious enough to see on a scan, a blood test, or a clinical work-up.
It is much less equipped to value subtle but meaningful changes in function before the picture becomes obvious.
That is a problem.
Because wearables are now everywhere. Millions of people are walking around with devices that track HRV, sleep, heart rate, stress markers, and recovery trends. Most of that data is ignored, misunderstood, or treated as interesting but not particularly useful.
I think that is short-sighted.
No, a wearable should not override clinical judgement. No, HRV should not be treated as a standalone diagnostic tool.
But dismissing these patterns entirely makes even less sense, especially when they can provide early evidence that a person’s system is under unusual and sustained stress.
At the very least, this kind of data should help direct attention.
If a patient presents to emergency with symptoms, and they also happen to have a wearable showing a sharp deviation from their normal baseline across HRV, sleep, resting heart rate, and recovery metrics, that should at least be considered useful context.
Because medicine is often trying to answer two questions at once:
What is wrong?
How concerned should we be right now?
Wearable data may not always answer the first question. But in some cases, it may help sharpen the second.
That feels especially relevant in busy emergency settings, where time is limited, context is fragmented, and clinicians are often forced to make decisions quickly.
Too often, the healthcare system is really a sick care system. It waits for the problem to become undeniable before action is taken.
By then, the window for preventative action may already be closing.
*I’m incredibly grateful to the people who helped me through this. I’m grateful for the GP who listened, for the specialists who followed through, for the hospital staff who cared for me once I was admitted, and for a healthcare system that ultimately provided ten days in hospital and weeks of home-based treatment through Medicare at no cost.
But I’m also left with a hard truth.
The system let me down at the point where early context mattered most.
And that delay came at a cost that I'm still paying.
Reserve Capacity May Be The Deeper Lesson
Looking back on the whole experience, I was lucky.
Not lucky that it happened.
Lucky that my system had enough reserve to tolerate it for as long as it did.
A spinal infection is not a trivial issue. It is not a minor setback, and it is not the sort of thing you want left untreated while you try to push on with normal life. In my case, the infection was present for roughly three weeks before antibiotics were started. When you say that out loud, it should make anyone stop and think. That is a long time for a serious internal problem to be brewing without targeted treatment.
The reason I say I was lucky is because I do not think every organism would have handled that the same way.
I believe my baseline health mattered.
Before this happened, I was not coming from a position of chronic dysfunction, severe metabolic illness, or years of complete physical neglect. I had a strong training background, a decent engine, a solid history of physical adaptation, and a system that, broadly speaking, had been exposed to stress and taught to recover from it over many years. That does not make anyone invincible, and it certainly does not make them immune to infection. But it may give them a greater margin for error when life turns sideways.
That margin matters.
In performance language, you could think of it as reserve capacity.
The healthier and more resilient the organism is before a major insult, the more room it may have to compensate when something goes wrong. That reserve does not eliminate the threat, but it may buy time. It may allow the body to hold the line for longer. It may blunt the speed at which function collapses. And in situations where diagnosis and treatment are delayed, that extra time can matter a lot.
I suspect that was true in my case.
That is one of the big lessons here.
Good health does not guarantee protection from disease or bad luck. But it can improve your odds of withstanding the hit, recognising when something is wrong, and recovering once the right intervention begins.
For years, I have spoken about training, nutrition, recovery, and mindset as investments in your future self. This experience sharpened that belief. Because when everything is going well, health can feel abstract. It can feel like a performance asset, an aesthetic goal, or a quality-of-life bonus. But when something genuinely serious happens, health is no longer abstract. It becomes your buffer. Your reserve. Your ability to stay in the fight long enough to get help.
Practical Takeaways: What Everyday People Should Know
You do not need to be a professional athlete to benefit from HRV.
You do not need to be obsessed with data, and you do not need a sports science degree to use it well.
But you do need to stop looking at it in isolation.
If you wear a wearable, pay attention to trends such as:
HRV dropping below your normal range for several days
resting heart rate climbing above baseline
sleep quality deteriorating
stress readings staying elevated
energy, mood, and training tolerance falling away
a general sense that something is not right
One of these on its own may be noise. Several of them together, especially when they persist, are a signal.
That does not mean panic. It means pay attention.
It means asking better questions. It means adjusting your training load, recovery, and lifestyle inputs. And if the pattern is strong enough, it means seeking medical attention with more urgency and more confidence that something real may be unfolding.
Final Thoughts
HRV is not magic. It is not a diagnosis. It is not a substitute for common sense, coaching judgement, or medical assessment.
But it can be a very useful early warning sign.
A canary in the coalmine.
A signal that the organism is no longer operating within its normal range. A prompt to look closer. A reminder that recovery data is not just about training readiness, but about the broader state of the system itself.
Sometimes that signal reflects a tough week, poor sleep, or accumulated stress.
And sometimes it reflects something far more serious.
The skill is knowing the difference between reacting emotionally to the number and responding intelligently to the pattern.
That is the real value of HRV.
If you track HRV, recovery, sleep, or readiness data, use it wisely. Do not worship it, and do not ignore it.
Learn your baseline. Watch the trends. Respect the patterns. And when the system keeps telling you something is off, do not be too quick to explain it away.
Sometimes the canary is only reacting to a hard week.
And sometimes it is warning you that something deeper is going on.
Want the free HRV Cheat Sheet?
If you want a practical guide to understanding what your recovery data is actually telling you, grab the free HRV Cheat Sheet below.





Comments